One million tons.
That's how much waste medical practices, research facilities, and dental offices generate. The World Health Organization reports that each day, high-income countries can produce a pound of hazardous waste per hospital bed. To safely get rid of the blood, fluids, and infectious matter, you need a complete disposal program. Without it, human health and nature could suffer, and heavy fines would follow.
What Could Go Wrong?
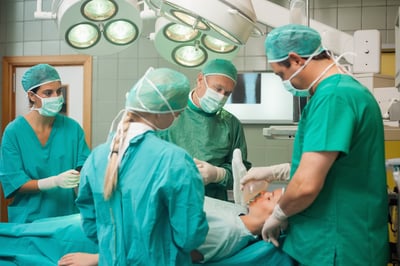 Many risks can come from biohazard waste disposal. In addition to environmental contamination, medical and laboratory workers are in danger of infection from bacteria, viruses, and parasites.
Many risks can come from biohazard waste disposal. In addition to environmental contamination, medical and laboratory workers are in danger of infection from bacteria, viruses, and parasites.
Also, with each event come fines; a citation from OSHA alone may cost $12,675 to $126,749 per violation. With such costly outcomes, you should address the challenges of biohazard waste disposal head-on.
Challenge 1: Knowing Your Regulations
Unlike other hazardous wastes, medical waste disposal is not controlled by the EPA's Resource Conservation and Recovery Act. Don't get confused, though. RCRA does regulate medical pharmaceutical (chemical) wastes, and it did publish a guideline manual 25 years ago. The Center for Disease Control, which protects the nation's health, also offers information about safe handling of infectious waste. Laws, however, come from OSHA, DOT, and individual states.
Occupational Safety and Health Administration: Under the Bloodborne Pathogens Standard, OSHA sets regulates controls, work practices, training, hazcom standards, and storage. It does not, however, regulate the final disposal of biohazard wastes.
Department of Transportation: When shipping biohazard waste, you must adhere to the Hazardous Materials Regulations. The DOT requires the shipper of the waste to follow guidelines for classification, markings, packing, shipping papers, and security.
State Departments of Health or Environmental Protection: The final disposal laws for biohazardous waste often come from state agencies. If there is an overlap between state and federal rules, though, you should follow the more stringent rules.
Challenge 2: Environmental Impacts of Disposal
Waste, when not controlled, can contaminate the environment. Biohazardous waste must be treated (to render it non-hazardous) and/or stored for final disposal. Treatment comes from chemicals, incineration, or autoclaving, all of which may provide risks of their own. Faulty processes could fail to remove the hazard, making the treatment useless. For example, incineration only works for certain wastes and only at extreme temperatures. If something goes wrong, it can pollute the air with a toxic, cancer-causing ash. Autoclaved (steamed) items may still be a hazard if the steam is not hot enough. Biohazard wastes are supposed to end up in a sanitary landfill; if they don't, they might find a way to public drinking water.
What You Need To Know
Biohazard Waste Classifications
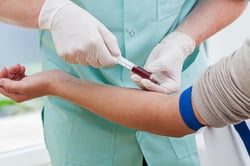 Solids. Items, except sharps, that were touched by or used on bodily materials (tissue, blood, body fluids) from humans or animals. Examples include latex gloves, bed sheets, and Petri dishes.
Solids. Items, except sharps, that were touched by or used on bodily materials (tissue, blood, body fluids) from humans or animals. Examples include latex gloves, bed sheets, and Petri dishes. - Liquids. These include liquids and semi-liquids made up of wasted blood, semen, or other bodily fluids.
- Sharps. Any object that has been exposed to harmful material that can puncture skin or a plastic bag.
- Pathological. Infected organs, tissues, or other remains removed from humans or animals.
DOT Classifications
- Category A: infectious items that could cause harm to those who were exposed to it. Those that affect animals are identified with the number UN2900. Those that affect humans are UN2814.
- Category B: An infectious substance that is not likely to cause harm to others due to exposure. These are given the ID number UN3373.
Proper Labeling and Storage
You must collect and store material as it becomes waste right away, so you are required to keep approved receptacles nearby. OSHA's Bloodborne Pathogens Standard regulates containers used to hold biohazardous material. For example, waste must be stored in red plastic biohazardous bags that are held in rigid, closing containers. Containers holding liquids must be leak-proof and inside of a second containment. All sharps require containers that can't be punctured. Sharps that fit the biohazardous criteria should also be clearly labeled.
It is a good idea to schedule regular pickups for this waste. Before leaving the building for final medical waste removal, it must be packed and labeled as required by the DOT in 49 CFR 173. Infectious materials must be triple contained. The original storage vessel is surrounded by a secondary packaging with a complete list of contents. These, finally, should be enclosed in a rigid, impenetrable, leakproof outer shell.
What happens next?
The outer package must be marked and accompanied by shipping papers in order to meet the DOT Hazardous Materials Regulations. After your waste manager logs your waste in a manifest, they will then haul it off to be treated, recycled, or stored in a sanitary landfill. When all workers receive the proper training and follow regulatory systems, the entire process can remain incident free.



Comment